Poop Pill
- Kellie Wong
- 3 min read
Fields covered: Microbiology, Microbiome, Microbiome-based therapy
Related Articles:
§ ![]() Clostridium difficile: Bacteria That Can Infect People Taking Antibiotics
Clostridium difficile: Bacteria That Can Infect People Taking Antibiotics
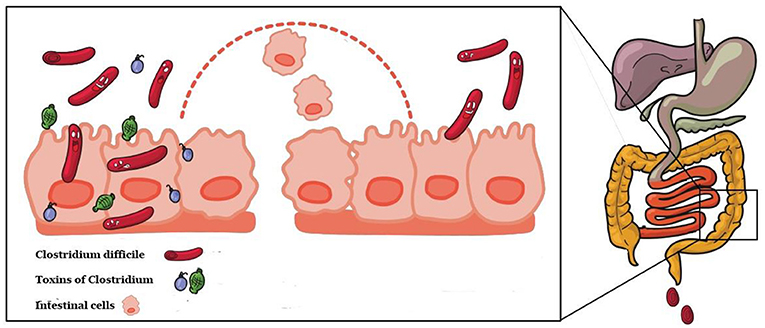
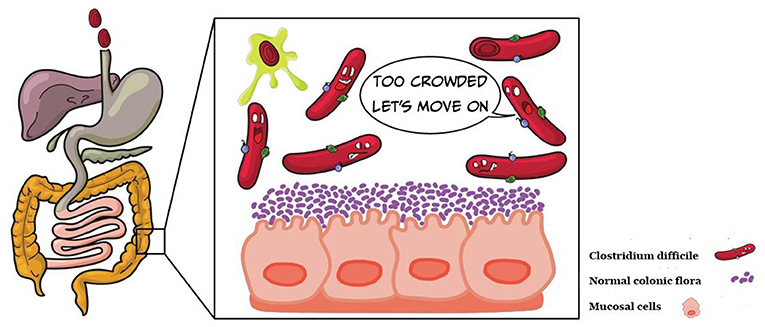
Together with many other microorganisms, C. difficile can exist harmlessly in our gut1. They are known collectively as the gut microbiome. The balance of the gut microbiome, or the relative composition of each microorganism in relation to other microorganisms in the gut, is intricately linked to our health2. Generally, a balanced gut microbiome translates to good health, while an unbalanced one is often associated with diseases2. When our gut microbiome becomes unbalanced3, such as following the use of antibiotics (which kills bacteria aimlessly, killing both the beneficial and harmful ones), it makes room for nasty, disease-causing bacteria – such as C. difficile – to replicate and colonize the gut. Thereafter, C. difficile can release toxins, and in large enough numbers, to stimulate inflammatory pathways and diarrhea4 (Figure 1).
You may have encountered the feisty Clostridium difficile (C. difficile) at some point – when you were on the loo!
C. difficile, a type of bacteria, is one of the most common causes of antibiotic- and healthcare-associated diarrhoea1. C. difficile infection usually follows antibiotic treatment or by ingestion of C. difficile spores1. Spores are the means by which the bacteria spread. But just because you’ve ingested C. difficile spores doesn’t automatically mean you will get diarrhoea. So what turns this bacteria from a harmless microbe into a stomach-twisting menace?
Besides C. difficile-associated diarrhoea, many other diseases, such as neurodegenerative diseases, cardiovascular diseases, and metabolic diseases, are associated with imbalances in the gut microbiome7. Microbiome-based therapy, such as this pill containing purified microbiome from human stool samples, is a field with much promise!
A quick and easy introductory video on gut microbiome: https://cdhf.ca/health-lifestyle/introducing-the-human-gut-microbiome-animation/
References
- Vedantam G, Clark A, Chu M, McQuade R, Mallozzi M, Viswanathan VK. Clostridium difficile infection: toxins and non-toxin virulence factors, and their contributions to disease establishment and host response. Gut microbes. 2012 Mar 1;3(2):121-34.
- Olvera-Rosales LB, Cruz-Guerrero AE, Ramírez-Moreno E, Quintero-Lira A, Contreras-López E, Jaimez-Ordaz J, Castañeda-Ovando A, Añorve-Morga J, Calderón-Ramos ZG, Arias-Rico J, González-Olivares LG. Impact of the gut microbiota balance on the health–disease relationship: The importance of consuming probiotics and prebiotics. Foods. 2021 Jun;10(6):1261.
- Clostridium difficile (C. diff) [Internet]. nhs.uk. 2022 [cited 4 July 2022]. Available from: https://www.nhs.uk/conditions/c-difficile/
- Burke KE, Lamont JT. Clostridium difficile infection: a worldwide disease. Gut and liver. 2014 Jan;8(1):1.
- Servick K. Pill derived from human feces treats recurrent gut infections [Internet]. Science.org. 2022 [cited 4 July 2022]. Available from: https://www.science.org/content/article/pill-derived-human-feces-treats-recurrent-gut-infections
- Feuerstadt P, Louie TJ, Lashner B, Wang EE, Diao L, Bryant JA, Sims M, Kraft CS, Cohen SH, Berenson CS, Korman LY. SER-109, an oral microbiome therapy for recurrent Clostridioides difficile infection. New England Journal of Medicine. 2022 Jan 20;386(3):220-9.
- Chen Y, Zhou J, Wang L. Role and mechanism of gut microbiota in human disease. Frontiers in cellular and infection microbiology. 2021:86.
Other Briefs
“Do you not think that there are things which you cannot understand, and yet which are; that some people
see things that others cannot?”